In 2017, however, the average age of mothers giving birth in all OECD countries was 30. Just under half (44%) of all live births in England and Wales in the same year were to mothers aged 30 while the average age of women giving birth to their first child in South Korea was 31.
MY WORLD OF TRUTH
Tuesday, 1 September 2020
How far can female fertility be extended?
“Its one of nature’s great inequities,” says Dagan Wells, professor of reproductive medicine at the University of Oxford. He is referring to the progressive, and largely irreversible, decline in female fertility from the age of 35 years onwards.
Men also experience a decline in their baby-making ability as they get older, but this fall in fertility tends to start later and occur much more slowly than in women. The fertility rate for men tends to begin falling around the age of 40-45 years old.
But when exactly does a woman’s fertility start declining? And when does that decline result in the end of natural fertility?
For millennia, women have been getting pregnant and bearing children in their teens and early 20s. Up until the 1960s, the average age of a regular, working woman, at the birth of her first child, was between 17 and 19 years – not much different from the Krapina Neanderthals, living in Northern Croatia 30,000 years ago, whose fossilised remains suggest gave birth to their first child at 15 years of age.

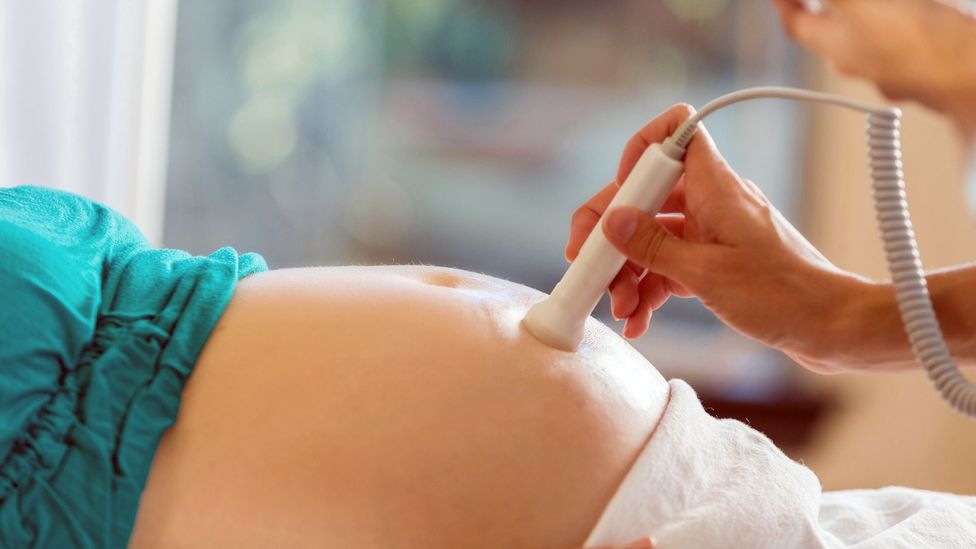
Fertility treatments and the ability to freeze eggs has allowed more women to have children later than was possible in the past (Credit: Science Photo Library)
But what does this mean in the context of the ticking clock of female fertility?
Numbers matter
For decades, scientists have associated the decline in female fertility with the age-related decrease in the number of eggs contained within a woman’s ovaries. Each, if fertilised, has the potential to grow into a baby.
Unlike men, whose reproductive organs produce millions of fresh sperm on a daily basis, women are born with all the eggs that they will ever possess. Moreover, this number steadily declines as a woman ages: from one million eggs at birth to 300,000 by puberty, 25,000 by the age of 37 and 1,000 by the age of 51. Of all these, however, just 300 to 400 eggs with baby-making-potential – normally just one a month – will mature and eventually be released from a woman’s ovaries through ovulation across her entire life. For reasons not yet fully understood, the rest undergo a natural process of degeneration and will never be ovulated.
While egg counts decline as women age, so does the quality of the chromosomes and the DNA contained within each egg
Most girls begin menstruating between nine and 13 years of age, but their ovaries don’t start releasing eggs until a least a year or two later. Simple mathematics would suggest a woman’s egg supply would then typically exhaust itself around 33 years later. And in most women, fertility does indeed tend to cease up to eight years before the onset of menopause, which for American women is around the time of their 51st birthday.
While such crude calculations do not take the natural variability that can exist between women into account, or the time windows during which ovaries might release more than one egg in a month, or months in which no egg is released at all, they can give a rough estimate of just how long the female fertility timeline can be.
A more precise estimate of a woman’s egg count, also known as “ovarian reserve”, can be obtained by measuring the level of hormone called anti-Mullerian hormone (AMH) in a woman’s blood. We now know that AMH, produced by the ovaries of fertile, adult women, plays a vital role in the metamorphosis of an immature egg cell into a mature, hopeful egg, complete with the all the biological prerequisites to create a healthy baby. Better functioning ovaries, with larger egg stores, produce more AMH. Levels of the hormone decline as the timeline of female fertility progresses – average levels in 30 to 35 year olds are roughly two-thirds that of younger women while levels in women aged over 45 years are a quarter of those seen in women in their 20s.

When they are born, women's ovaries already contain all the eggs they will ever produce – around a million on average (Credit: BBC)
Andrea Jurisicova, an embryologist at the Lunenfeld-Tanenbaum Research Institute of Mount Sinai Hospital, has spent years studying the mechanisms that underpin the decline in female fertility with age, and investigating what can be done to slow this. Her research has found that ovarian reserve is genetically regulated but that a woman’s life experiences – such as stress, exposure to radiation or toxic chemicals and even those from when she herself was in the womb – determine egg numbers in later life.
Quality matters
But female fertility isn’t just about the quantity of eggs. Quality matters too, and is much more technically challenging to assess than egg numbers. While egg counts decline as women age, so does the quality of the chromosomes and the DNA contained within each egg.
“Chromosomal abnormalities in human eggs are extremely common,” says Wells. “It’s not something that should be considered to be a particularly abnormal situation, and in most cases its something that all women, even young women, will have in their eggs at a low level but that level increases with advancing age.”
For a woman in her 20s, a quarter of her eggs may be expected to have chromosomal abnormalities, this increases to up to 40% for a woman between 30 and 35, and “goes up simply exponentially from there on”. Beyond the age of 35, the frequency of these chromosomally abnormal eggs increases by 0.5% per month, so that for a woman in her early 40s up to three-quarters of her eggs will have chromosomally abnormalities.
An egg with too many or too few chromosomes, broken or damaged chromosomes will often fail to develop properly
Having chromosomal abnormalities in her eggs doesn’t necessarily mean a woman is infertile, but they do mean that more of her menstrual cycles will produce eggs that are less likely to produce a viable baby.
Chromosomes are bundles of tightly coiled DNA that hold the genetic information needed for an organism to develop. A human egg contains 23 chromosomes – the half of your genetic code that comes from your mother – which needs to combine with the 23 chromosomes from your father’s sperm to develop into a viable embryo. An egg with too many or too few chromosomes, broken or damaged chromosomes will often fail to develop properly. In some cases a baby can still be born with chromosomal abnormalities, as happens with Down’s Syndrome.
But most chromosomal abnormalities tend to be lethal to the extremely young embryo, resulting in the embryo failing to implant in the lining of the wound or a very early miscarriage, often between five and eight weeks of pregnancy.
While the risk of chromosomal abnormalities is known to be higher in the eggs of older women, a recent European study found that the level of chromosomal abnormalities is also high in younger women too – from 13 into their early 20s. The findings suggest that female fertility timeline follows a n-shaped pattern, with peak fertility observed in the mid-20s and lower levels of fertility both in very young and older women.
Older mothers may face greater risks during pregnancy, labour and delivery, but there are problems associated with older fathers too (Credit: Getty Images)
Elsewhere in the egg, faulty mitochondria – the tiny power stations that provide energy for our cells and which we all inherit from our mothers – can also be a problem in older women. Studies have shown that up to half the eggs of women who are older than 35 carry mutations in their mitochondrial DNA, compared to a third of the eggs in younger women.
“An egg needs a threshold of about 40,000 mitochondrial DNA copies to make an embryo,” says Jurisicova.
For Wells, the evidence is clear.
“The rate of decline accelerates around the age of 35 and the vast majority of women are essentially infertile by the time they reach 45,” says Wells. “Importantly, this is years, maybe even a decade, before menopause. Everyone expects to be a little less fertile when you are older, but the extent of that decline takes a lot of people by surprise.”
It would be wrong to focus only on female fertility. Some studies have shown that sperm quality also declines with age in men, starting in their 20s. Sperm mobility – the ability of it to swim around – has been found to decline by around 0.7% every year while the sperm of older men carry more mutations in their DNA. Older fathers also pass on more mutations to their children than mothers do from their eggs.
Best egg
“The human egg is a remarkable and unusual cell, it’s the biggest cell in the body, and has a unique feature,” says Wells. He is referring to the egg’s ability to stop halfway through its growth and remain in a state of suspended animation for years, even decades, until it is eventually ovulated. His research suggests that it is the egg’s ability to hold its chromosomes in a stable configuration during this period of hibernation that governs its ability to make an embryo and a baby.
While there may be little that science can do to change the number of a woman will have during her life, there are ways to improve egg quality
Jurisicova’s work adds another piece to the puzzle. Her work suggests that human eggs undergo a process of growth and maturation within the ovary for at least nine months before they are released during ovulation. “The quality of the egg released is the culmination of all the health and environmental influences on that growing egg over the past nine months,” she says. Stress, exposure to radiation or toxic chemicals during this time can have an adverse effects on the developing egg.
It is perhaps interesting that the duration of this incubation period – from when an egg emerges from hibernation and begins developing – uncannily resembles the number of months a baby spends within the womb before it is born. During this period of maturation, the egg develops the resources it will need should it be fertilised.
“The egg has to be extremely well resourced,” says Wells. “For the first three days following fertilisation the embryo doesn’t really make anything for itself – it doesn’t transcribe its genes, it doesn’t make proteins – its completely reliant on what the egg has provided for it. A more mature egg is more likely to be better resourced than a less mature one.”
While there may be little that science can do to change the number of eggs that nature (or genetics) decides a woman will have during her life, Wells and Juriscicova agree there are ways to improve, or rescue, egg quality. Adopting a healthy lifestyle, exercising regularly, reducing stress and making sure that health problems such as hypothyroidism and other autoimmune conditions are well controlled can all help.
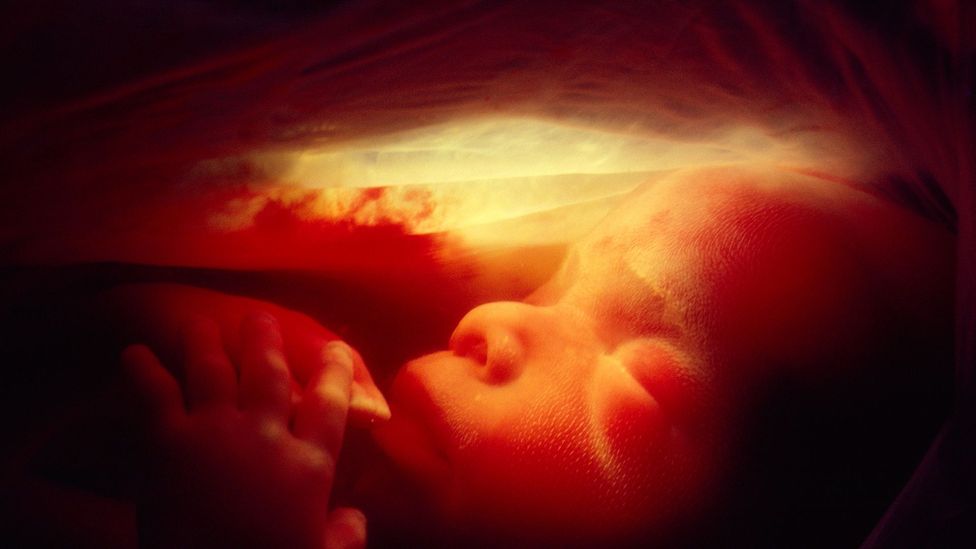
The range of factors pitched against an egg being fertilised and developing into a foetus make childbirth seem all the more incredible (Credit: Science Photo Library)
Jurisicova recently found that giving female mice the antioxidant coenzyme Q10 delivers promising results – the mice that received the supplement produced better quality eggs with more properly aligned chromosomes and better mitochondrial function. They were also more successful in producing live babies, than the mice that did not receive the supplements. The results are, however, yet to be replicated in humans.
The journey, not the destination
Mothers don’t just need to contend with their fertility as they get older, but also greater risks during pregnancy, labour and delivery. The First and Second Trimester Evaluation of Risk (Faster) trial, a US study funded by the US National Institute of Child Health and Human Development (NICHD), looked at the health records of over 36,000 women. They found mothers over 40 were two to three times more likely to experience health problems during pregnancy including diabetes and high blood pressure. They were twice as likely to experience bleeding from their placentas, have a caesarean delivery and to lose their baby later on in pregnancy.
The children of older first-time mothers who are 40 years and above also have an increased risk of health problems at birth, such as low birth weight and congenital abnormalities. They also have a 50% increased risk of being born preterm and, perhaps consequently, are at increased risk of requiring neonatal intensive care after birth.
But this is still only one half of the equation. Older fathers also bring additional health risks for their children. Babies with older fathers are more likely to be born prematurely, have a lower birth weight and higher risk of seizures. Some studies have also linked increasing paternal age to a greater risk of conditions such as autism and ADHD where the father is over the age of 40, but the evidence remains inconsistent.
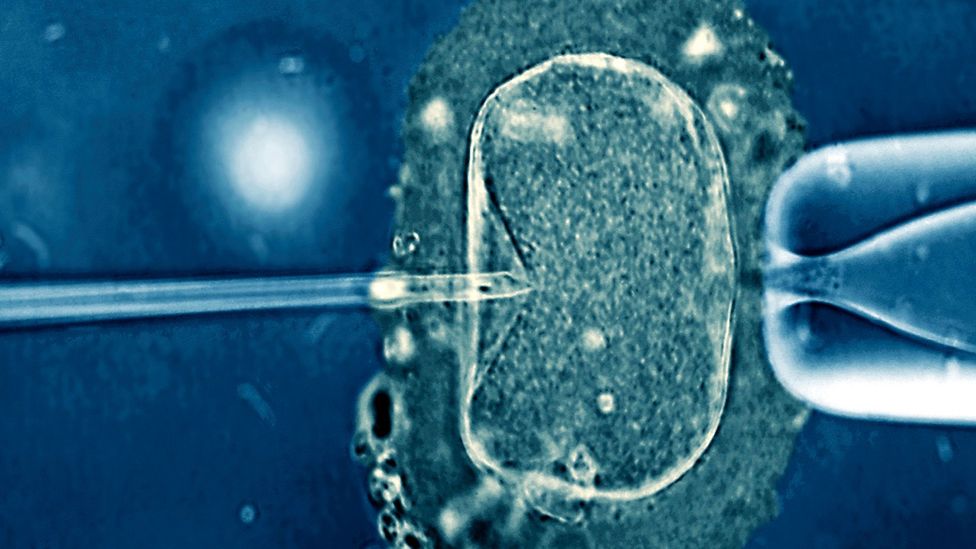
Scientists are developing new techniques to identify the best eggs for use in IVF treatments (Credit: Science Photo Library)
Is it possible to extend female fertility and for how long? As is often the case, where nature creates inequity, science attempts to level the playing field. In September last year, Erramatti Mangamma, a 74-year-old from southern India become the world’s oldest first-time mother, delivering twin baby girls conceived via In Vitro Fertilisation (IVF) after 57 years of infertility. Three years ago, 72-year-old Daljinder Kaur, from north India, gave birth to a son after nearly five decades of marriage and two unsuccessful IVF attempts.
The significant advances in reproductive medicine over the past decades have greatly increased the safety, success, accessibility and affordability of artificial reproductive techniques. Approximately 230 babies are born in the UK each year to women aged 50 and over while 9% of all first-time mothers in the US were aged above 35 in 2014.
But as we have seen, these techniques are still limited to a degree by the age of the egg. This is, not least, because of the effects of ageing on the DNA, but also because older eggs have been exposed to environmental toxins for a longer amount of time. It is possible, of course, for women to undergo IVF using a donated egg from a younger woman. Nearly all fertility clinics across the world now also offer women an option to store their eggs, frozen in time, until she is ready for them to be thawed, fertilised and transplanted into her womb.
“The difficulties experienced with older women trying to have children is not related to the uterus but to the egg, and chromosomal abnormalities are at the heart of that,” says Wells. “The egg is the seed rather than the soil. Many of the very early steps in human development are determined by what the egg provides.”
With the help of technologies like pre-implantation genetic testing, Wells and his fellow embryologists are developing ways of identifying the best eggs that can be used in IVF treatments. Other techniques such as mitochondrial replacement therapy are also helping mothers with defects in their eggs give birth to healthy children.
But while science is making commendable steps to help prolong the ticking clock of female fertility, it may not ever be possible to keep it going indefinitely. The decline of natural female fertility is as inevitable as it is universal.
posted by Davidblogger50 at 00:27

0 Comments:
Post a Comment
<< Home